
Atopic dermatitis (AD) also known as eczema, is a chronic skin issue marked by red and dry skin patches, commonly on the arms, legs, and face (though they can appear in other places as well.)
It is noteworthy that in people with darker color skin the dry areas instead of just being shades of red can be red-brown or a purple-gray color. Let’s explore more about this itchy skin condition in this blog, including symptoms, causes, and treatments of atopic dermatitis.
What is Atopic Dermatitis?
According to the dictionary, the word “atopic” refers to an allergic reaction that occurs in a part of the body that didn’t come into contact with the allergen.
Really when we use the word “atopic” or “atopy” in medicine we refer to a genetic tendency to develop an allergic disease like “hay fever” (allergic rhinitis), asthma, or eczema. It is in reality a skin disorder that causes inflammation, itching, and dry skin patches.
It can affect anyone, adults, teenagers, toddlers, and babies. However, according to the American Academy of Dermatology, it mostly develops in childhood. It sometimes clears up as the child grows older while in other cases it may come and go for the rest of the life in the form of atopic eczema flareups.
What Causes Eczematous Dermatitis?

Atopic dermatitis is caused by skin barrier dysfunction. Many connections in the skin make it an excellent barrier to the outside world. If one of these connections is not working correctly then this barrier does not work like it should and irritants from the outside can easily penetrate into the body and cause inflammation.
Some of the common factors that may disrupt a skin barrier dysfunction are
Genetics
If a person has a family history of atopic dermatitis, hay fever, asthma, or allergies then they are more prone to developing the conditions.
The gene variation in a person’s body can make it difficult for the skin barrier to retain moisture properly and provide protection against irritants leading to dryness and itching. This is usually when the gene lacks an epidermal protein known as filaggrin.
Bacteria
An excess of bacteria known as Staphylococcus aureus on the skin can also cause a weakened skin barrier. The overproduction of this bacteria leads to the loss of helpful bacteria on the skin (that protects your epidermis), which can cause symptoms like itching, allergic rashes, and inflammation.
Immune System
The immune system is responsible for protecting the body and skin against outside bacteria, viruses, and illness. However, a weak or overactive immune system can make your skin more prone to developing skin disorders like eczema, psoriasis, and dermatomyositis.
Food Allergies
Hypersensitivity towards certain food items can trigger a flare-up or further exacerbate the existing condition. Some common food allergens are:
- Eggs
- Wheat
- Soy
- Peanuts
- Milk
Environmental Triggers
Causes of flare-ups of atopic dermatitis can vary from person to person but some common factors are:
- Harsh soaps and other cleansers
- Perfumes and dyes commonly found in skincare products
- Rough fabrics
- Stress
- Mold, pollen, and animal dander
- Dry skin
- Low humidity
- Tobacco smoke
- Sweating and heat
- Cold, dry air
- Skin infection
- Extended showers and baths at elevated temperatures
Avoiding these triggers can help reduce flare-up frequency. But wait — there’s more!
Atopic Dermatitis Symptoms
If you are wondering what does atopic dermatitis looks like here is your answer. It is characterized by dry, scaly patches on skin, and red rashes that flare up for some time, go away, and then reappear sporadically.
In some cases, other symptoms may accompany the rash, including:
- Raised bumps that weep when scratched
- Swelling and Skin inflammation
- Blister rash
- Lichenification ( thickening of skin)
- Scaly skin
- Extreme dryness (xerosis)
- Itchy skin (pruritus)
- Skin discoloration
- Cracked, bleeding skin (most commonly caused by scratching)
It may also cause red rashes on skin which may appear as pink or red on lighter skin tones and purple or brown on darker skin tones. The symptoms usually appear in the following areas
- Hands
- Feet
- Arms
- Legs
- Face
- Neck
- Eyelids
The location of the symptoms may differ in different age groups, so let’s discuss how atopic eczema may change as a person grows old.
Infantile Atopic Dermatitis
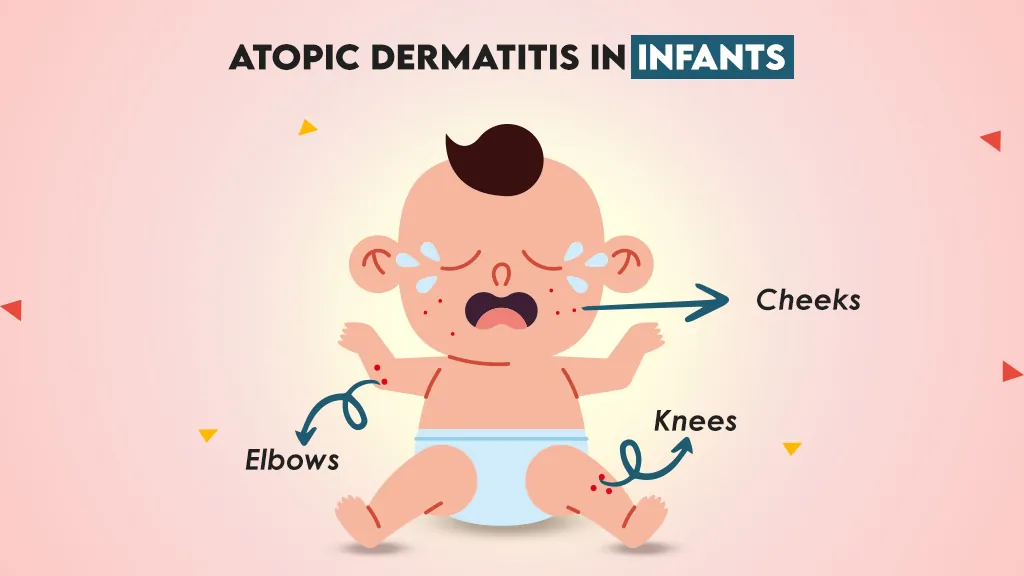
When infants or babies less than the age of 2 experience this condition it is known as early-onset atopic dermatitis. It mostly appears on the
- Cheeks
- Knees
- Elbows
- Back of the hands
Many of the atopic eczema cases that start at this age resolve during childhood. However, in some cases, the condition may stay for a lifetime and flare up from time to time.
Atopic Dermatitis in Children
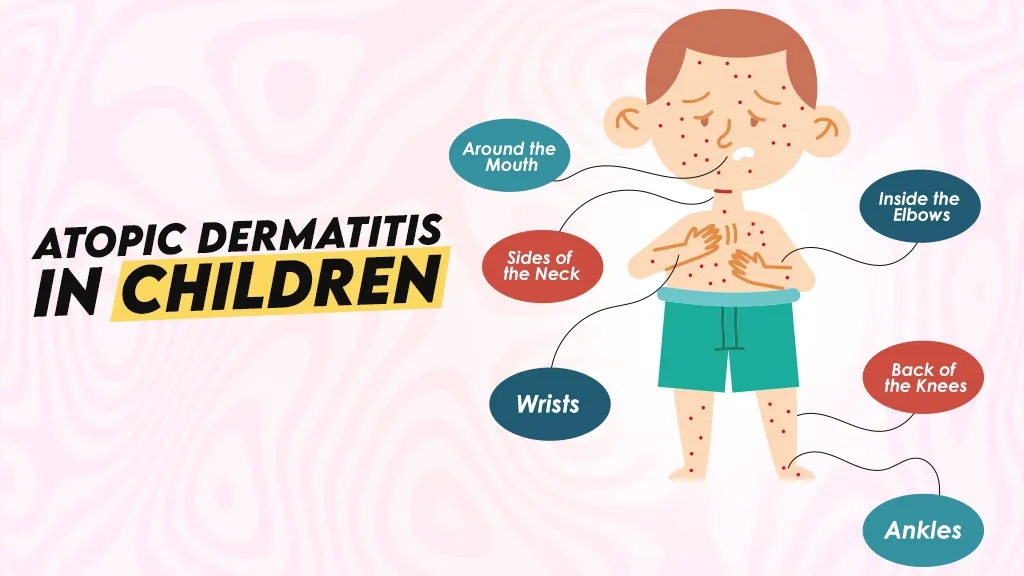
As the child grows older the location and severity of the conditions may also change. As the baby starts crawling they can develop atopic dermatitis on the outside of the elbows and knees. As the child grows older the rash tends to move to the inside of the elbows and the knees, and on the wrists and ankles.
As it is difficult to control toddlers and children from scratching their skin. The itching may become worse and lead to severe lichenification, skin damage, infections, and scarring. The rashes may also appear on the neck which can be an answer if you are wondering why is my kid’s neck red.
Atopic Dermatitis in Adults
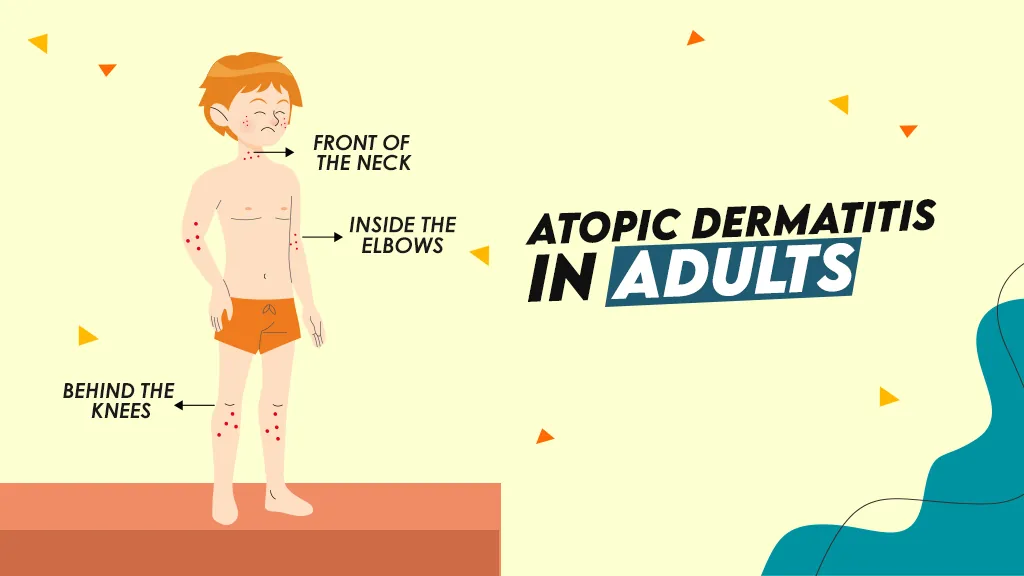
From adolescence through adulthood the rash continues to be found in the folds of the arms and legs, on the wrists and ankles, and is also found on the neck and eyelids. Eczema in adults is more common on the hands classified as hand eczema. Which is usually caused by occupational and domestic work.
Most people develop this skin disorder in childhood but some people may experience it for the first time in adulthood. Adults and children can also develop it around the nipples or breast which is classified as nipple eczema.
There are different terms used for when this condition develops in adults
- Adult-onset: the condition develops for the first time in adulthood.
- Late-onset: symptoms appear after puberty
- Senile-onset: symptoms appear in people older than 60 years old.
How Common is Atopic Dermatitis?
The condition is more common than you think. It is likely if one of the parents has a health history of eczema the child is 50% at risk of developing it. And if both parents had the skin issue then the risk increases to 80%.
According to the National Eczema Association, it affects around 9.6 million children, and 16.5 million adults annually in the United States. Approximately 1 out of 10 individuals are likely to develop or experience this skin disease once in their lifetime.
Atopic Dermatitis Vs Eczema
Many people consider eczema and atopic dermatitis as the same. Even doctors use these terms interchangeably. Every atopic dermatitis is eczema. But not every eczema is atopic dermatitis.
Eczema is a broad term used to describe skin conditions that cause itching and dryness. Atopic dermatitis is one of its subtypes. There are various different types of eczema and each one may have the iconic symptoms of itching and dryness but can be a little different from one another.
Some other common types are:
- Contact dermatitis
- Seborrheic Dermatitis (cradle cap in babies)
- Dyshidrotic Eczema
- Discoid Eczema (nummular eczema)
- Juvenile Plantar Dermatosis
- Varicose Eczema
- Asteatotic Eczema
The most prevalent types in these are atopic and seborrheic dermatitis, which is very common in babies as cradle cap. If your baby is also suffering from cradle cap then try using a medicated cradle cap shampoo and if desired, a cradle cap brush to reduce the scaling, flaking, and future build-ups.
Atopic Dermatitis Vs Contact Dermatitis
These are the two most common types of eczema experienced in adults and children. The difference between both conditions is that atopic dermatitis can appear anywhere on the body and it can flare up from time to time.
While with contact dermatitis you will experience a flare-up only when the skin comes in contact with a certain irritant or allergen and the rashes will only appear on that specific area of the skin.
The rashes in atopic dermatitis are usually dry and scaly and with contact dermatitis the rash can include blisters and weeping lesions.
Atopic Eczema Treatment

There is no permanent cure for this skin issue. However, taking proper care of the skin can help soothe the symptoms and prevent the occurrence of future flare-ups.
Atopic Dermatitis Selfcare
Keep the Skin Clean
It is important that you keep your skin clean. Due to the skin barrier dysfunction, the skin becomes more vulnerable and has a higher risk of developing infections and other complications.
- Take a bath every day with an eczema shampoo and body wash.
- Use lukewarm or cool water to wash the skin.
- Use an eczema cleanser that is fragrance-free, paraben-free, and sulfate-free.
- After washing, pat dry your skin, as excessive rubbing can exacerbate the condition.
Moisturize Often
Skin with atopic dermatitis can become excessively dry leading to cracks and bleeding. Which is why it is important to keep it moisturized as much as possible.
- Moisturize your skin with an eczema cream at least twice daily.
- Use a hypoallergenic moisturizer that does not further irritate your skin.
- Remember to moisturize your skin within 3 minutes after taking a bath. The skin is able to retain more moisture at that time.
Don’t Scratch
Scratching should be avoided at all costs with any type of eczema. Here is why–scratching the skin leads to a never-ending itch-scratch cycle. This cycle can make your condition worse. Intense scratching can damage your skin and cause other issues like skin infections.
Use Gentle Products
If you are experiencing eczema or atopic dermatitis it is important that you use mild, gentle products with low pH on your skin. Products that contain harsh chemicals like fragrances, artificial dyes, and sulfate (SLS, SLES) can further exacerbate the condition.
Use a shampoo, body wash, face wash, cleanser, and moisturizer that are free from these skin-irritating chemicals and contain natural ingredients like licorice root extract, glycerin, and Provitamin B5.
Manage Stress
Sometimes stress can trigger a flare-up or make your condition worse. You can easily manage stress-related eczema and atopic dermatitis through counseling, exercise, yoga, meditation, and doing the things that you love.
Right Clothing
You may love that wool black dress of yours, but do you know certain types of fabrics can irritate your skin and exacerbate your dermatitis? This is why it is important to choose loose-fitting clothes made of lightweight and breathable material like cotton.
For washing your clothes use a gentle detergent that is free of fragrance and any harsh chemicals. Harsh detergents can trigger contact dermatitis and make you suffer from two different types of eczema at the same time.
Use Humidifier
Some people may notice that their symptoms get worse during winter. This is because the skin loses more moisture due to the cold, dry air. You can use a humidifier in your house, office, or room if you think that the dry air is making your skin dry.
Humidifiers can help eczema by adding moisture to the air and protecting the skin from getting dry.
Atopic Dermatitis Therapy
In some severe atopic dermatitis cases, the doctor may prescribe therapies to soothe the symptoms.
This treatment is typically only done at the suggestion of a physician. It helps when the rash and itch is severe–especially in children. These dressings can be placed overnight to provide relief while sleeping. Corticosteroid ointment or cream is applied to the affected area, it is then covered with a wet dressing followed by a covering of dry cloth or gauze. Again a doctor should be consulted before applying this type of dressing.
- Light Therapy
If topical medication and self-care are doing no good to your condition then this therapy may be advised by the doctor. In this, the affected area is exposed to artificial ultraviolet A and narrow band ultraviolet B to make the condition better. This is also known as phototherapy.
- Counseling
Atopic dermatitis often causes physiological issues like depression, anxiety, and stress due to itching and sleep deprivation. Then counseling can help those people get rid of the issues and make their life quality better.
Medications for Atopic Dermatitis
Medications are prescribed by doctors to control and soothe itching, irritation, and redness. These medications are often in the form of cream, ointment, lotion, and sometimes oral medications.
Make sure that you use these only when prescribed by a doctor and for the period they advised. Some common medications are
- calcineurin inhibitor
- Antibiotic pills
- Antihistamines
- Cyclosporine
- Azathioprine
- Prednisone
- Injectable biologics
Other Complications
People who experience atopic dermatitis are more prone to developing other allergies such as seasonal allergies. When a person develops asthma, atopic eczema, or hay fever (allergic rhinitis) one after the other it is known as the “atopic march.”
Some other complications that can accompany the skin condition are:
- Bacterial skin infection
- Viral skin infection
- Stress, anxiety, and depression
- Neurodermatitis
- Sleep disruption
- Eye problems like Conjunctivitis and Blepharitis.
Not all of these complications may be experienced. They may develop in some cases while in others they may not. If you are experiencing any of these conditions along with eczematous dermatitis it is best to consult a doctor for proper treatment.
Key Takeaways
- Atopic dermatitis is a chronic skin condition.
- Inflammation, itching, dryness, and scaling skin are its most prominent symptoms.
- It is not contagious.
- The symptoms may vary a little in different age groups
- There is no permanent cure for atopic dermatitis, but it can be managed with a proper eczema skincare routine.
FAQs
- About
- Latest Posts
- WhatToExpect Mentioned Happy Cappy Shampoo as the Best Medicated Shampoo For Cradle Cap - September 29, 2025
- Parents.com Mentioned Happy Cappy Shampoo in the List of 10 Best Shampoos for Babies and Kids of All Hair Types - September 29, 2025
- Chain Drug Review Covers Happy Cappy’s CVS Launch Nationwide - August 27, 2025
Does atopic dermatitis get worse with age?
The answer to this question depends from person to person. In some cases, the condition may get better and resolve as the child grows older. For others, this condition may become a lifelong issue that appears again as flare-ups and gets better after some time.
What is atopic dermatitis caused by?
The main cause that leads to atopic dermatitis is skin barrier dysfunction. The skin loses more moisture and becomes more prone to be infected by outside irritants. Some other factors that can cause this dysfunction are genetics, environmental triggers, and allergies.
What is the difference between atopic dermatitis and contact dermatitis?
Atopic dermatitis can appear anywhere on the body and at any time. But contact dermatitis is only caused when the skin comes in contact with an irritant or allergen. It usually appears only on the specific area that was touched.
Can atopic dermatitis go away permanently?
There is no permanent cure for atopic dermatitis. It all happens inside the body and can not be controlled. However, you can manage its symptoms by taking proper care of the skin.
What other conditions are mistaken for atopic dermatitis?
There are various other conditions that may look similar to this issue such as
Psoriasis
Neurodermatitis
Nummular eczema
Acne
Rosacea
Vitiligo
Best eczema cream for atopic dermatitis?
The eczema cream to moisturize your skin is the one that is free from harsh chemicals like
Fragrance
Dyes
Paraben
Sulfate
Soy
Lanolin
It contains more natural ingredients and has a low pH level. These moisturizers can help soothe the itching and redness, restore the skin barrier, and maintain a normal pH level of skin.
Suggested Products
Buy today
-
 3 Step Baby Skincare Routine Bundle for Baby Acne-Prone and Sensitive Newborn Skin with FREE Beanie Brush
$30.60 / 3 weeks – $34.00
3 Step Baby Skincare Routine Bundle for Baby Acne-Prone and Sensitive Newborn Skin with FREE Beanie Brush
$30.60 / 3 weeks – $34.00
-
 Happy Cappy Baby Bath Bundle for Neonatal Acne Skin with Beanie Brush, Medicated Fragrance-Free Shampoo and Body Wash
Happy Cappy Baby Bath Bundle for Neonatal Acne Skin with Beanie Brush, Medicated Fragrance-Free Shampoo and Body Wash
$23.99Original price was: $23.99.$22.99Current price is: $22.99. -
 Happy Cappy Neonatal Baby Acne Shampoo and Body Wash Fragrance-Free Gentle Care for Newborn Skin
$26.60 / 3 weeks – $109.08
Happy Cappy Neonatal Baby Acne Shampoo and Body Wash Fragrance-Free Gentle Care for Newborn Skin
$26.60 / 3 weeks – $109.08
Also Available at



Recent Posts
- WhatToExpect Mentioned Happy Cappy Shampoo as the Best Medicated Shampoo For Cradle Cap
- Parents.com Mentioned Happy Cappy Shampoo in the List of 10 Best Shampoos for Babies and Kids of All Hair Types
- Chain Drug Review Covers Happy Cappy’s CVS Launch Nationwide
- Trend Hunter Mentions Happy Cappy Brand Launch in Over 6,800 CVS Pharmacies Nationwide
- MSN Mentioned Happy Cappy Skincare Line’s Primary Products Launch In CVS across the U.S




